Emergency Dentistry
Gum Disease Explained Without the Scare Tactics
If you have ever noticed bleeding when you brush, persistent bad breath, or gums that look a little puffier than usual, it is easy to shrug it off and hope it goes away. The tricky thing about gum disease is that it often does seem to “come and go” at first. That is part of what makes it so easy to ignore.
Here is the more helpful way to think about it: gum disease is not a sudden event. It is a slow shift in the health of the tissues that support your teeth, and it usually starts quietly. The earlier you understand what is happening, the easier it is to stop it before it causes permanent damage.
This article breaks down gum disease in a way that actually makes sense, so you can spot the early signs, understand the progression, and know when it is time to come in for a professional assessment at Akemi Dental Specialists.
The short version of gum disease
Your gums are not just “pink skin.” They are a living barrier that seals around each tooth. When plaque and bacteria sit along the gumline long enough, your body responds with inflammation. If that inflammation stays unresolved, the seal loosens, deeper bacteria move in, and the supporting structures, including bone, can begin to break down.
Gum disease generally moves through two main stages:
- Gingivitis: inflammation of the gums (often reversible).
- Periodontitis: deeper infection and breakdown of support (not fully reversible, but manageable).
Common signs people notice, and the ones they do not
Some symptoms are obvious. Others are easy to miss or explain away.
Signs you might notice:
- Bleeding when brushing or flossing
- Swollen or tender gums
- Bad breath that keeps returning
- Gums that look red or “puffy”
- A bad taste that comes and goes
Signs that can sneak up on you:
- Teeth looking longer (gum recession)
- Slight tooth shifting or spaces forming
- Food packing between teeth more than it used to
- Increased sensitivity near the gumline
- A change in your bite that feels subtle at first
One important point: pain is not a reliable early warning sign. Many people have active gum disease with very little discomfort.
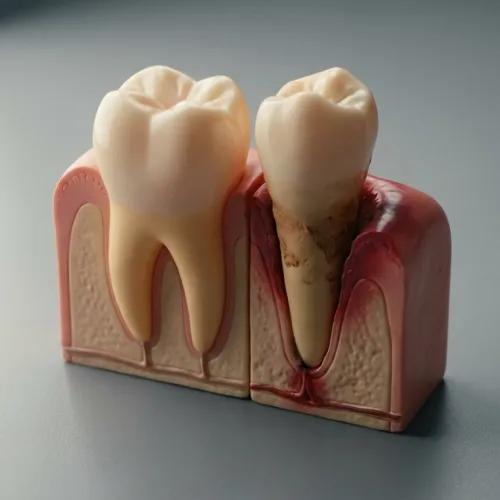
What actually happens beneath the gums when gum disease begins?
Even if your teeth look clean, there is a whole ecosystem living at the gumline. When plaque is not removed thoroughly, it hardens into tartar (calculus), and bacteria become harder to disrupt with brushing alone.
Here is what is happening under the surface:
- Plaque builds at the gumline. It is sticky, bacterial, and forms quickly.
- The gums become inflamed. This is your immune system reacting to the bacteria.
- The gum seal starts to weaken. Healthy gums fit snugly around the tooth. Inflammation makes that seal less stable.
- A pocket can form. This creates a deeper space where bacteria can thrive.
- The bacterial mix changes. Early plaque bacteria are different from the bacteria that thrive in deep pockets. As the pocket deepens, the environment becomes more oxygen-poor, and more aggressive bacteria can dominate.
Think of it like this: early gum disease is not just “dirty gums.” It is your body being stuck in an inflammatory cycle. Over time, that cycle starts affecting the structures that hold teeth in place.
Why bleeding matters: Bleeding is often the first visible sign that the gum tissue is irritated and inflamed. It is not simply “brushing too hard.” In many cases, it is your gums saying, “I am not healthy right now.”
How does gingivitis turn into periodontitis?
Gingivitis is the early stage, and it is the stage where we have the best chance of a full reset with good home care plus professional cleaning.
Gingivitis becomes periodontitis when inflammation becomes ongoing and deeper bacteria take hold. At that point, the issue is no longer only at the gum surface. It involves the attachment structures underneath.
Here is the progression in a practical way:
- Gingivitis begins at the edges. The gums swell and bleed more easily because the tissue is inflamed.
- The attachment starts to loosen. The gum tissue and fibers that hold the tooth snugly can begin to pull away.
- Pockets deepen. Deeper pockets collect bacteria, tartar, and inflammatory byproducts.
- The body starts breaking down support. In periodontitis, the immune response can contribute to destruction of the supporting bone and ligament around the tooth.
- Teeth become less stable over time. This can show up as shifting, looseness, or changes in bite.
Why this matters: periodontitis is not just “worse gingivitis.” It is a different stage where bone support can be lost, and lost bone does not simply grow back on its own.
Risk factors that can speed up the shift from gingivitis to periodontitis include:
- Smoking or vaping
- Diabetes or blood sugar instability
- Dry mouth (from medications, mouth breathing, dehydration)
- Hormonal changes (pregnancy, menopause)
- Chronic stress and poor sleep
- Genetics and family history
- Clenching or grinding (can worsen damage once inflammation exists)
None of these mean gum disease is inevitable. They simply mean you may need a more proactive plan.
Can bone loss start before noticeable gum symptoms appear?
Yes, and this is one of the biggest misunderstandings about gum disease.
Bone loss can begin quietly, especially if:
- You do not bleed much (some people do not bleed easily).
- You brush regularly but miss key areas where tartar accumulates.
- The problem is happening more in the back teeth where it is harder to see.
- Inflammation is present but mild enough that you do not feel pain.
Also, gum disease is not always dramatic in the early stages. You might only notice:
- Slight gum recession
- Mild sensitivity
- A little more bad breath than usual
- Floss that sometimes smells “off”
How do we detect early bone loss and periodontitis?
At Akemi Dental Specialists, we look at several clues together:
- Pocket measurements around each tooth
- Bleeding and inflammation patterns
- Tartar buildup location
- X-rays to evaluate bone levels and changes over time
- Tooth mobility and bite changes when relevant
This is why waiting for “serious symptoms” can backfire. By the time teeth feel loose, the disease is often advanced.
What you can do at home that actually helps
Home care matters, but it has to be the right home care. The goal is to disrupt plaque at the gumline consistently.
Focus on these habits:
- Brush twice daily for a full two minutes. Angle the bristles toward the gumline, not just the tooth surface.
- Clean between teeth daily. Floss, interdental brushes, or a water flosser can help. Consistency matters more than the tool.
- Do not “avoid” bleeding gums. Gentle cleaning helps them improve. Avoiding the area lets plaque mature and inflammation persist.
- Use an antibacterial rinse if recommended. Some cases benefit from short-term medicated rinses, but they are not a replacement for cleaning.
- Watch for dry mouth. Sip water, chew sugar-free gum, and ask about solutions if medications are causing it.
A simple checkpoint: If you have bleeding when brushing or flossing for more than a week, that is not something to ignore. It is a reason to get evaluated.
What professional treatment looks like, and why it works
Gum disease treatment is not about “scraping harder.” It is about removing what you cannot fully remove at home and reducing the bacterial load below the gumline.
Depending on what we find, treatment may include:
- Professional cleaning to remove plaque and tartar buildup
- Deep cleaning (scaling and root planing) when pockets and deeper buildup are present
- Localized antibiotic therapy in certain cases
- Periodontal maintenance visits more frequently than standard cleanings
- Targeted recommendations for tools and technique based on your specific anatomy
- Referral or collaborative periodontal care if advanced support is needed
The goal is to stop progression, reduce inflammation, and help you keep your natural teeth healthy for the long term.
When to schedule an appointment
You do not need to wait for a crisis. In fact, gum disease is one of those problems that is easier and less expensive to address early.
Consider booking an evaluation if you have:
- Bleeding when brushing or flossing
- Bad breath that returns quickly
- Gum recession or teeth that look longer
- Sensitivity near the gumline
- A family history of gum disease
- Diabetes, dry mouth, or smoking history
- A feeling that something is “off” even if you cannot pinpoint it
If you suspect gum disease, schedule an appointment with Akemi Dental Specialists. We will evaluate your gum health, measure pockets, review X-rays if needed, and walk you through a clear plan to get things back on track before bone loss becomes the headline of your story.