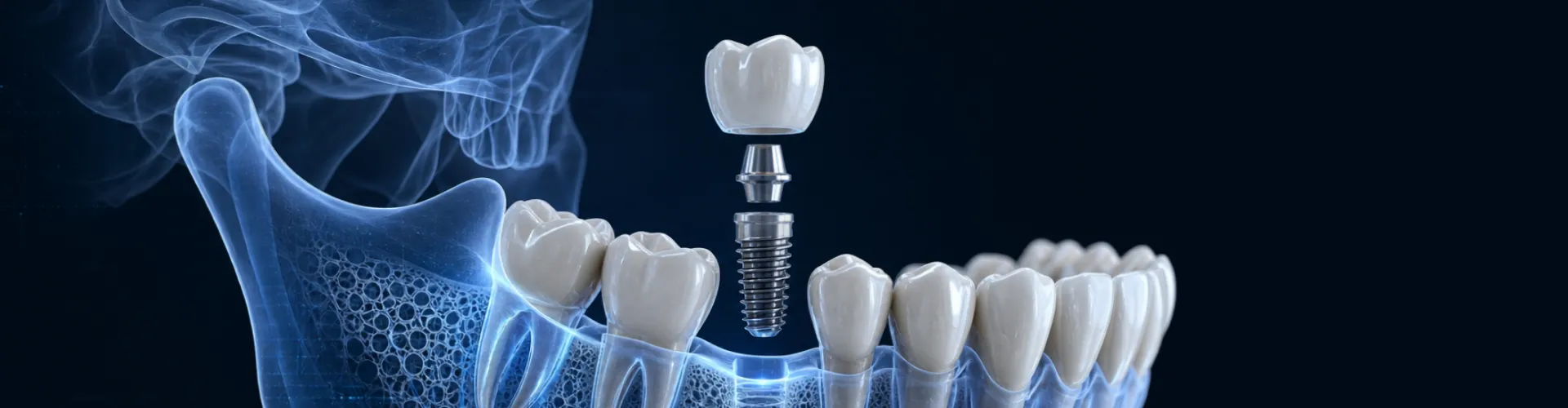
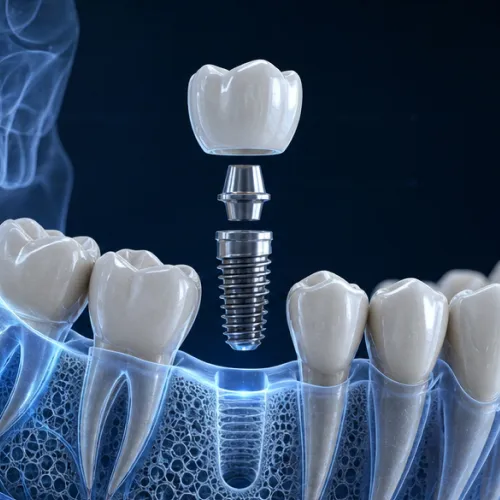
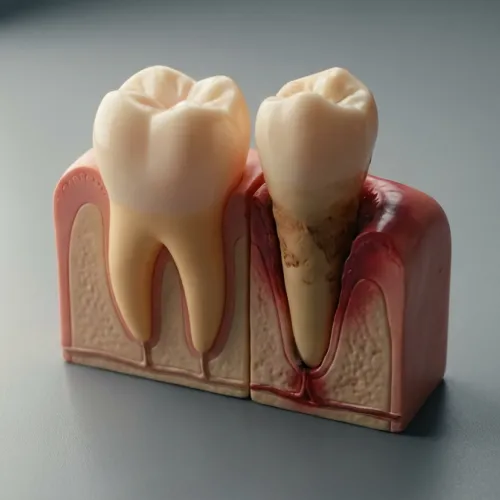
Restorative Dentistry, Implant Dentistry
Autoimmune Disease, Bone Grafting, and Dental Implants: What Actually Determines If You're a Candidate
Having an autoimmune disease doesn't automatically disqualify you from dental implants — but your medications, inflammatory status, and bone volume matter far more than your diagnosis alone. Understanding how these factors interact gives you a real roadmap to candidacy.
Your Medications May Be the Real Barrier — Not Your Disease
This is the distinction I see patients miss most often. For Encino-area patients, someone researches "Can I get implants with lupus?" and finds a binary yes/no answer. But the condition itself rarely tells the whole story. What actually threatens osseointegration — the process where bone fuses structurally to the implant — is the pharmacological profile of your treatment.
Consider the drug classes most commonly prescribed for autoimmune conditions:
Corticosteroids (prednisone, hydrocortisone): Long-term use predisposes patients to secondary osteoporosis and impairs bone healing. High-dose glucocorticoids alter the inflammatory response that is essential for osseointegration to proceed normally.
Biologic DMARDs (TNF-α inhibitors like adalimumab or etanercept): These suppress the immune pathways that also orchestrate wound healing and early implant integration. They increase infection susceptibility during the surgical window.
Bisphosphonates and antiresorptives: These carry risk of medication-related osteonecrosis of the jaw — a serious complication that can develop after oral surgery.
The concept of a "drug holiday" — temporarily pausing certain medications in coordination with your rheumatologist — can create a safer surgical window. This isn't something to attempt unilaterally. It requires interdisciplinary planning, but it's a legitimate strategy that shifts otherwise marginal candidates toward viability.
Research published in PMC confirms that implant survival rates remain generally high even among autoimmune patients on immunosuppressants, with implant losses occurring predominantly before prosthetic loading — meaning the surgical and early healing phase is where optimization matters most. According to the Mayo Clinic, health conditions that affect bone healing are among the primary factors evaluated before any dental implants surgery is scheduled.
Timing Surgery Around Your Inflammatory Load
Beyond medication management, when you have the surgery is as consequential as whether you have it. Autoimmune diseases cycle through exacerbations and remissions. Operating during a flare dramatically increases the risk of early implant failure.
One practical tool I discuss with medically complex patients is C-Reactive Protein (CRP) testing. CRP is a blood marker that rises with systemic inflammation. Elevated CRP at the time of implant surgery signals that your immune system is in an "attack state" — actively mounting inflammatory responses that can interfere with osseointegration and increase the likelihood the implant is treated as a foreign body rather than integrated as a functional root.
A pre-surgical optimization window of roughly 60 days is worth pursuing: working with your physician to achieve disease remission, reducing inflammatory dietary triggers, and confirming blood markers are within a stable range before scheduling surgery. This isn't about perfection — it's about stacking the odds in your favor during the critical healing period.
A systematic review via Cleveland Clinic-adjacent research found that despite the heterogeneity of autoimmune conditions studied, dental implant survival rates were comparable to those in the general population when proper maintenance and long-term follow-up were maintained. Scrupulous oral hygiene and monitoring — not avoidance — were the common determinants of success. Learn more about habits and pro tips to maintain your dental implants to set yourself up for long-term success.
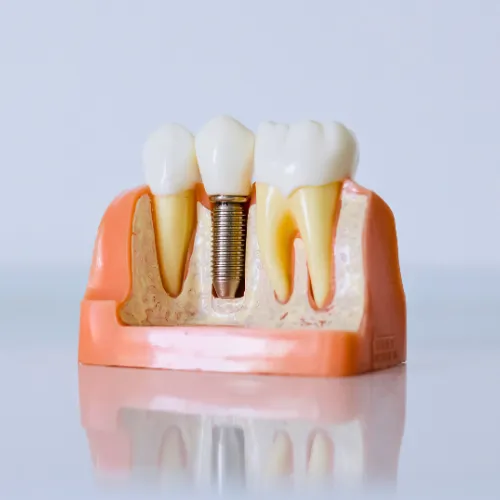
When Bone Volume Is the Problem: Graft-Free Alternatives
Not every barrier is immunological. Many patients — with or without autoimmune disease — present with insufficient jawbone volume to support conventional implants. Long-term tooth loss, periodontal disease, and the bone-thinning effects of corticosteroids all accelerate alveolar ridge resorption.
The standard response has historically been bone grafting, which rebuilds density before implant placement. Grafting works well, but it adds months to the timeline and introduces additional surgical sites and healing demands — a real concern for patients who are immunocompromised.
What's less commonly discussed are zygomatic and pterygoid implants. These are specialized, longer implants that bypass the dental arch entirely, anchoring instead into the dense bone of the cheekbone (zygoma) or pterygoid plates. For patients with severely resorbed maxillae who have been told they're "not candidates," this approach can provide fixed teeth without a single bone graft — often within 24 hours of implant placement.
This isn't the right solution for every case. But for the right anatomy, it eliminates the graft-healing variable entirely, which is particularly valuable when immune function is a concern.
According to the American Academy of Periodontology, full-mouth implant solutions are designed to integrate with available jawbone and preserve what remains — making alternative anchoring strategies clinically relevant when conventional bone volume is absent.
For cases where some bone is present but inadequate, grafting remains a highly predictable option. A Healthline overview of mini dental implants also notes that smaller-diameter implants require less bone density, offering another pathway for patients with moderate bone loss who want to minimize surgical complexity.
So Can Anyone Get Dental Implants?
The honest answer: most people can, but not without individualized evaluation. The checklist that matters isn't just "do you have an autoimmune disease" — it's the full clinical picture.
Key variables I assess include:
- Disease stability: Is the autoimmune condition currently in remission or active flare?
- Medication profile: Which drug classes are involved, and is a surgical window achievable?
- Bone volume: Is there sufficient density for conventional implants, or are alternative approaches needed?
- Inflammatory markers: Are blood values consistent with a healing-state physiology?
- Oral hygiene capacity: Implants require consistent home care; conditions that cause dry mouth (like Sjögren's syndrome) or limited mouth opening require specific protocols.
General health, age, and smoking status all factor in as well. Smoking significantly impairs healing and remains one of the strongest modifiable risk factors for implant failure regardless of systemic health status. Our advanced technology supports precise evaluation of all these variables before any treatment is recommended.
The goal of my evaluation process is not to find reasons to exclude patients — it's to identify what needs to be optimized before we proceed. For the majority of motivated patients, including those with autoimmune conditions, a pathway to implants exists.
Schedule a Consultation at Akemi Dental Specialists in Encino
If you've been told you might not be a candidate for dental implants — or if you're managing an autoimmune condition and wondering where to start — I'd encourage you to get a proper evaluation before accepting that answer.
At Akemi Dental Specialists in Encino, I work with medically complex patients throughout the San Fernando Valley to develop implant plans that account for the full clinical picture. That means coordinating with your physicians, reviewing your medication profile, and evaluating bone volume with precision imaging before making any recommendations. Our endodontics and periodontics specialists collaborate closely to ensure every aspect of your oral health is addressed as part of your treatment plan.
Contact our office to schedule a consultation.
Medical disclaimer: This article is intended for informational purposes only and does not constitute medical or dental advice. Individual circumstances vary. Consult a qualified dental professional and your physician before making any decisions about dental treatment.